
CASE REPORT
published: 24 May 2022
doi: 10.3389/fnhum.2022.893830
Frontiers in Human Neuroscience | www.frontiersin.org 1 May 2022 | Volume 16 | Article 893830
Edited by:
Siegfried Othmer,
EEG Info, United States
Reviewed by:
James H. Lake,
Western Sydney University, Australia
Meike Wiedemann,
Owner of Neurofeedback
Clinic, Germany
Fabian Bazzana,
University of Turin, Italy
*Correspondence:
Regula Spreyermann
Specialty section:
This article was submitted to
Brain Health and Clinical
Neuroscience,
a section of the journal
Frontiers in Human Neuroscience
Received: 10 March 2022
Accepted: 15 April 2022
Published: 24 May 2022
Citation:
Spreyermann R (2022) Case Report:
Infra-Low-Frequency Neurofeedback
for PTSD: A Therapist’s Perspective.
Front. Hum. Neurosci. 16:893830.
doi: 10.3389/fnhum.2022.893830
Case Report: Infra-Low-Frequency
Neurofeedback for PTSD: A
Therapist’s Perspective
Regula Spreyermann
*
Praxis Dr. med. Regula Spreyermann, Basel, Switzerland
The practical use of a combination of trauma psychotherapy and neurofeedback
[infra-low-frequency (ILF) neurofeedback and alpha-theta training] is described for the
treatment of patients diagnosed with complex post-traumatic stress disorder (C-PTSD).
The indication for this combined treatment is the persistence of symptoms of a
hyper-aroused state, anxiety, and sleep disorders even with adequate trauma-focused
psychotherapy and supportive medication, according to the Guidelines of the German
Society of Psycho-Traumatology (DeGPT). Another indication for a supplementary
treatment with neurofeedback is the persistence of dissociative symptoms. Last but not
least, the neurofeedback treatment after a trauma-focused psychotherapy session helps
to calm the trauma-related reactions and to process the memories. The process of the
combined therapy is described and illustrated using two representative case reports.
Overall, a rather satisfying result of this outpatient treatment program can be seen in the
qualitative appraisal of 7 years of practical application.
Keywords: post-traumatic stress disorder (PTSD), neurofeedback for PTSD, neurofeedback combined with
psychotherapy, hyperarousal, trauma, C-PTSD
SETTING FOR THE TREATMENT OF PATIENTS WITH COMPLEX
POST-TRAUMATIC STRESS DISORDER USING
TRAUMA-FOCUSED PSYCHOTHERAPY AND NEUROFEEDBACK
For indications such as complex post-traumatic stress disorder (C-PTSD), a close interdisciplinary
collaboration is called for. In this case, a close collaboration between the psychiatric doctor’s
office with a focus on psycho-traumatology (Peter Streb, MD, Psychiatry and Psychotherapy,
Basel, Switzerland) and the office for psychosomatic medicine offers neurofeedback (Regula
Spreyermann, MD Internal Medicine, Basel, Switzerland).
In trauma-focused psychotherapy, Peter Streb works according to the Guidelines of the
DeGPT, the German Society of Psychotraumatology (https://www.awmf.org) with stabilization,
trauma confrontation, and processing including specific interventions such as Eye Movement
Desensitization and Reprocessing (EMDR) or Imagery Rescripting and Reprocessing
Therapy (IRRT).
The additional psychosomatic treatment includes psychoeducation, neurofeedback,
mindfulness training, imaginative therapy, and general support throughout the process and
with optimization of the conditions of living (
Lake, 2015).
Once a week, the effects of th e combined therapy, the condition of the patients, acute problems,
medication changes, and the overall process are discussed interdisciplinary between the doctor’s
offices. Based on this regular exchange, decisions are made with respect to changes in training

Spreyermann Neurofeedback and Psychotherapy for C-PTSD
protocol or shifting the focus to either more psychotherapy or
more neurofeedback or only on one of them. This happens either
because the objective has been reached or because it became clear
that the additional effect is insufficient.
INDICATIONS TO ADD NEUROFEEDBACK
TO TRAUMA-FOCUSED
PSYCHOTHERAPY IN THE TREATMENT
OF PATIENTS SUFFERING FROM C-PTSD
Patients are sent to an additional treatment with neurofeedback
when, despite intensive trauma-specific psychotherapy and
different medications, insufficient relief from the typical PTSD
symptoms has been achieved (
van der Kolk et al., 2016). In these
cases, infra-low-frequency (ILF) neurofeedback (Othmer, 2017),
followed by alpha-theta training (Othmer and Othmer, 2017), is
used as an additional treatment of choice (Lanius et al., 2015).
There are also cases where a trauma-induced chronic
dissociation hinders effective psycho-therapeutic trauma therapy,
as emotions cannot be perceived by the patient (Lanius and
Frewen, 2015). In these cases, neurofeedback ca n help to lead to
better self-awareness, greater mental stability, and improved self-
regulation, which then in turn makes it possible to work on the
trauma (
Gerge, 2020a).
PTSD SYMPTOMS AND WHAT MAKES IT
C-PTSD
The typical symptoms of PTSD are symptoms of chronic stress
induced by trauma. These symptoms include hyperarousal,
sleep disorders, panic attacks, nightmares, flashbacks, muscle
tension, fatigue, lack of concentration, emotional instability, and
depressive symptoms. One speaks of C-PTSD if the persistent
PTSD symptomatology has led additionally to personality
changes and emotional dysregulation according to the criteria
of the International Classification of Diseases 11th Revision
(World Health Organization, 2022), which are typically induced
by persistent traumatization during childhood (emotional or
sexual abuse or violence or neglect) or during adulthood
following torture, abuse, violence, or loss. The persons affected
show symptoms of constant h yperarousal of the stress syst em
with inner unrest, anxiety, panic, sleep disorders, nightmares,
exhaustion, depression, and obsessive-compulsive behavior.
There are also physical symptoms of chronic tension that are
chronic pain in the mus culoskeletal system, bruxism, dental
defects, and headache (
Cloitre et al., 2013). Due to disorders of
the immune system caused by an impaired release of cortisol,
there is a high prevalence of infections, irritable bowel, and
other conditions (Boscarino, 2009). As a consequence of the
physical and mental exhaustion, ADHD-like symptoms (Kimbrel
et al., 2017
) such as distractibility, concentration disorders, or
procrastination can occur, which additionally can have an effect
on working capacity. The presence of trauma, flashbacks, and
avoidance behavior confirms the PTSD diagnosis.
The personality changes that lead to the diagnosis of a C-PTSD
are negative thoughts about t h emselves and others, mistrust, and
avoidance of social contacts.
The criteria for the diagnosis according to ICD/DSM are
adapted over time. A current discussion is the concept of
developmental traumatization. If the trauma is severe and
diagnosed at a late stage, in most cases, specialized psychotherapy
and usual medicinal treatment are required. Neurofeedback
offers in this study a promising additional benefit (
van der Kolk
et al., 2020; Micoulaud-Franchi et al., 2021).
PRACTICAL STEPS IN THE TREATMENT
OF PATIENTS WITH C-PTSD
The first step in the whole process takes place in the
psychotherapy practice. There is the need for a proper first
interview to gain a perspective on the history a nd background
of the patient and to determine which problems have priority.
It may be necessary to react with pharmacotherapy in the first
instance (sleep medicine, antidepressants, or anxiolytics), or to
initiate help with acute psychosocial problems by contacting
other doctors, family, employers, or insurance. In a further step,
it is important to move deeper into the special t rauma therapeutic
methods such as Imagery Reprocessing and Rescripting therapy
IRRT (
Grunert et al., 2007) or Eye Movement Desensitization and
Reprocessing EMDR (Shapiro, 1995). However, in many cases, it
is necessary to pursue mental (Lanius et al., 2017) and somatic
stability as a priority before working on the real trauma, and this
can be achieved using the neurofeedback as an additional next
step (
Panisch and Hang Hai, 2020). So the patients are informed
about this possibility and assigned to the psychosomatic therapist
to initiate the training (Gerge, 2020b).
The patients are informed about neurofeedback as a method,
about gained experiences, and the expect ed i mprovement as well
the possibility, in which within the first 10–15 sessions ups and
downs may occur. Based on this information, the shared decision
is made whether neurofeedback therapy is started or not. The
patient gets informed, that an evaluation will take place after
10–20 sessions to consider, whether the treatment is sufficiently
supportive or not.
In a further step, the medical, the personal, and the
family histories are elaborated on, as well as the current
symptoms’ presentation before we start. The assessment of
the individually important symptoms is conducted using a
computerized symptom questionnaire by EEG Expert called
“Symptomtracking” (https://eegexpert.net). It helps to rate the
severity of the relevant symptoms on a scale from 0 to 10. In
the course of the neurofeedback treatment, the symptom tracking
is repe ated every 2–3 months to be able to track the progress,
but also to be able to see in which domain more focus has
to be placed. The neurofeedback protocol priority is adjusted
accordingly (
Reiter et al., 2016).
The principal electrode placement used for trauma resolution
is T4-P4, which can be complemented or if necessary, changed
to T 3–T4 in case of instabilities, according to the Protocol
Guide 2017 by Sue Othmer. During the initial period of finding ,
Frontiers in Human Neuroscience | www.frontiersin.org 2 May 2022 | Volume 16 | Article 893830

Spreyermann Neurofeedback and Psychotherapy for C-PTSD
the optimal response frequency (ORF) to address the existing
symptoms such as hyperarousal, sleep disorders, flashbacks,
nightmares, anxiety, or muscle tensions, especially in pa tients
with high instability, ups and downs, and undesired side effects
can occur during the session, or within hours or days after the
session. These effects mostly last only for a few hours up to 1 or 2
days, and they help us to find the ORF (
Wiedemann, 2020).
After the ORF is found, it is important to find an optimal
rhythm for the sessions. One session per week is typical for an
outpatient setting; however, a biweekly rhythm can be better
tolerated. Regularity is of great importance, as the training
induces a process t hat ideally should not be interrupted, at least
not in the first 2 months.
Within this process, indications for additional sensor
placements can arise. The symptom tracking helps to monitor the
long-term course and also helps the patient to see progress and
stay motivated. Weekly communic ation with the psychotherapist
is of great importance to optimize the process for the patient.
When sufficient stabilization of the patient is achieved, trauma
confrontation may become easier. In a further step, synchrony
protocols (both in t he ILF and in the alpha band) may be
incorporated into neurofeedback therapy as an additional self-
regulation strategy. Synchrony training can also serve as a means
to assess the readiness to undertake alpha-theta training to
support the psychological reprocessing of the trauma (Imperatori
et al., 2017).
CASE PRESENTATIONS
In the following, two representative cases are elaborated to
illustrate t h e clinical process.
Case 1
Case 1 is a 40-year-old female suffering from C-PTSD caused
by th e violent death of her mother when she was around
20 years old. Over the years, there was psychotherapy with
various therapists, followed by around 10 years of psycho-
trauma therapy. Due to the residual hype rarousal, massive
sleep dysregulation, and nightmares, neurofeedback therapy was
advised. Sustained daytime flashbacks and dissociation were
reported by t he patient. In fact, the patient acted entirely
emotionless and absent. The answers were purely rational. In
contrast to the posture of “not-being-noticeable,” the patient
reports massive emotions such as fury, grief, helplessness,
anxiety, and panic being dissociated felt for her like dizziness. I n
addition, she was plagued by massive headaches, stress-induced
skin reactions, and tinnitus. The prehistory is heavily loaded,
growing up in a family full of conflicts, violence both emotional
and physical, a depressive and suicidal father, and a mother full
of sorrow about her drug-addicted brother.
There had been three suicides in the immediate family and
among c lose friends—she herself lost a close friend when she
was 5 years old, and at the age of 10, someone committed
suicide directly in her presence. Since childhood, she suffered
from poor sleep, nightmares, and restlessness in sleep. She had
daydreams about being adopted and her true parents coming
to rescue her. She had been ridiculed at school about her
skewed teeth as well as by her father. She withdrew and felt like
belonging nowhere. As a teenager, there were suicidal thoughts,
binge eating, and many illnesses. In her early 20s, the mother
died in violent death, and the father is also now de ceased.
Anniversaries of the deaths always increase the trauma-induced
symptoms, despite the passage of time. Looking at her childhood,
there are many consecutive events that led collectively to t h e
severe traumatization.
Neurofeedback Training and Symptom
Tracking
Due to a high emotional instability and very noticeable mistrust
and skepticism, T4-P4 was trained in the beginning. This calmed
down the patient. However, it also led to heavy side reactions such
as mood swings. For this reason, T3-T4 was added after session
7. After 25 sessions, T4-Fp2 was added. This protocol targets the
affective domain more directly. Again, there were panic states,
which were treated with T3-T4 for a few sessions. Now she is back
to a treatment solely with T4-P4 and alpha-theta.
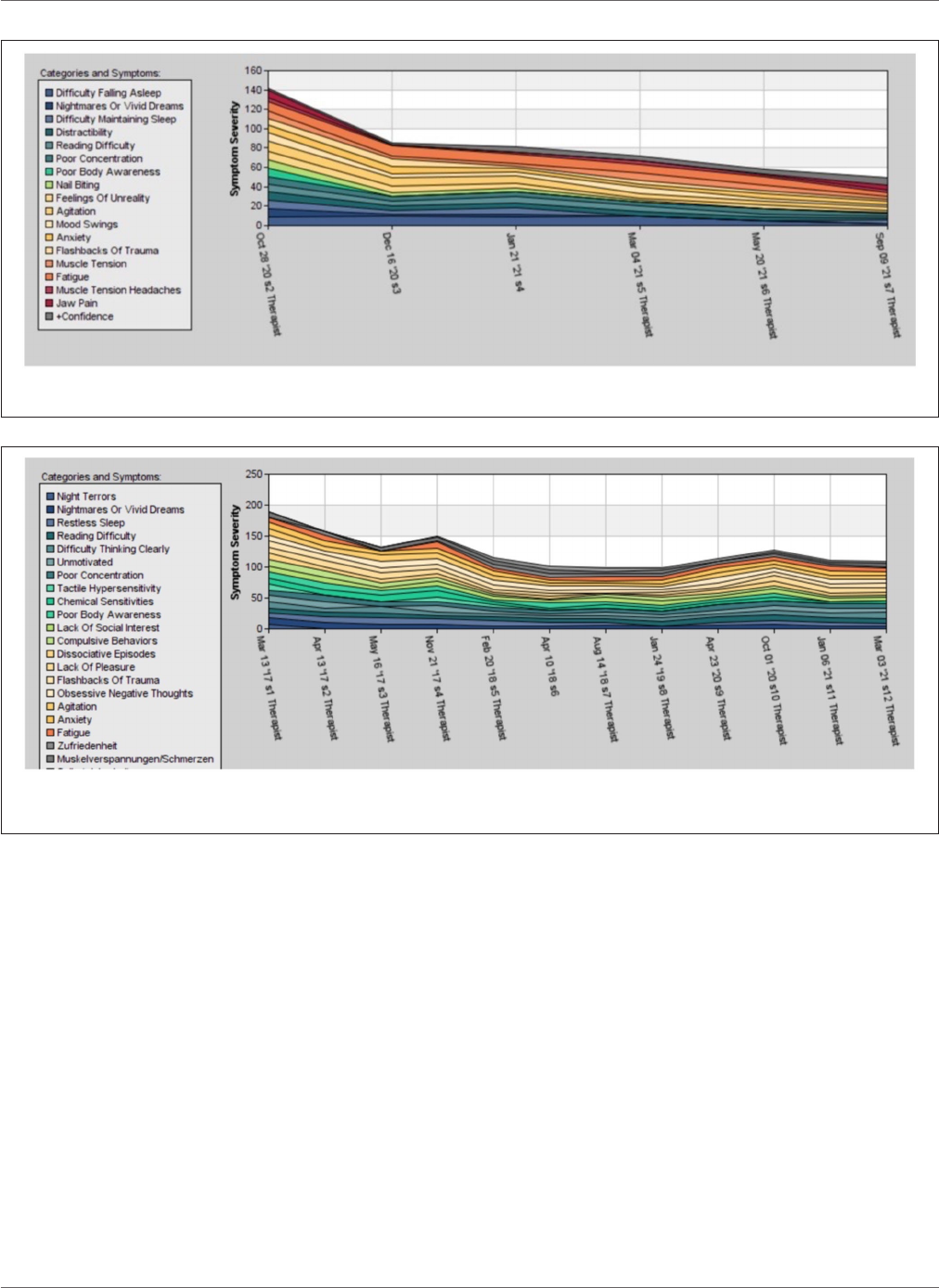
In Figure 1, the symptom tracking over the course of t ime for
the main symptoms is illustrated. The figure shows the steady
decline of symptom se verity to below 30% of the starting value,
over the course of 47 sessions. These symptoms had existed for
more than 20 years and could not be eliminat ed using medication
and psychotherapy.
In her own words, the patient describes herself as being back
to herself, back to the here and now, experiencing more placidity
and equanimity, and much better sleep.
The patient has now found her way back into life. She has
finished her dissertation, which she had started with panic attacks
and under hig h stress, without drama. She has found appropriate
employment. In the future, there is some work yet to be done
in terms of personal relationships. Due to the history of C-
PTSD and the ongoing personality changes, there is still a lot of
avoidance in her life, especially in terms of intimate relationships.
Case 2
Case 2 is the story of a 35-year-old female with C-PTSD. The
trauma dates back to early childhood. She was adopted as an
infant from the Far East by a German family with two children.
There was never the feeling of belonging to the family, and
this has persisted until the present. L ooking Asian while being
German, she has not found her real identity. This is one of the
reasons that she chose to start neurofeedback. The trauma was
triggered by continuous sexual abuse during primary school age,
but also from repeated relationships with heavy physical violence
by the partner, including brutal rape. As in the first case, the
trauma in this study cannot be traced back to a single event, but
rather to multiple insults. The patient suffers from permanent
and clear recognizable dissociation: her face looks mask-like and
her voice is t hin and unemotional. There is a steady twitching of
her eyelids due to flashbacks from violent scenes coming every
few seconds.
She has massive concentration and memory impairment,
making it impossible for her to work. Her sleep quality is
extremely poor; she awakes every few minutes; falling asleep
initially takes several hours. During the day, she is steadily
tired and exhausted. The only constant in her life has been her
daughter for whom she cares daily, cooks, goes horseback riding,
Frontiers in Human Neuroscience | www.frontiersin.org 3 May 2022 | Volume 16 | Article 893830
Spreyermann Neurofeedback and Psychotherapy for C-PTSD
FIGURE 1 | Time course of the different post-traumatic stress disorder (PTSD) symptoms of case 1 during 1 year of therapy, rated by the patient between 0 and 10.
FIGURE 2 | Development of the PTSD symptom during the 5 years of therapy in case 2. The ups and downs are the results of reduction of medicaments, life events
such as divorce, and re-traumatization.
and much more. She has been doing neurofeedback treatment
for around 4.5 years now. It stands out since the beginning of
the NF training that in combination with psychotherapy, there
is a steady and very positive development, one that is not always
visible in symptom tracking. The first noticeable improvement
was enhanced sleep, which helped her in her daily life. She
could deal better with her household and learned how to play
golf to enhance her concentration and be more outdoors. After
2 ye ars, she relates that she is less dissociated, “which is not
always ple asant.”
In a second step, she was able to reduce the extensive
psychiatric medication; first, the neuroleptics, then, the
antidepressants, and lastly, the sleeping pills. The only thing left
is sleep-inducing antidepressants.
In further progress, there was the separation from her
pill-addicted husband, where the relationship had been very
destructive. Another relationship ended with a physical attack.
After being on her own for several years, she is now in a new
relationship. Psychotherapy helps her to learn the fundamentals
of a trusting relationship. She has even successfully managed to
build up a company of her own.
ILF Training and Symptom Tracking
The symptom tracking in Figure 2 shows that in the beginning,
there is a quick improvement in symptom severity followed by
fluctuations. In October 2020, there was a relapse caused by the
terminal illness of her father.
The treatment of he avily traumatized patients is not
straightforward, as the relationship is often characterized in the
beginning by high levels of mistrust, avoidance, and need for
control in the frame of the attachment trauma. When sleep
improved, she reduced her medication, which led to instabilities
and t he need to find a new ORF.
For a while, she wanted to be independent and, therefore,
stretched the frequency of the meetings to a maximum. She only
came when sleep got worse again after around 3-4 weeks. Since
Frontiers in Human Neuroscience | www.frontiersin.org 4 May 2022 | Volume 16 | Article 893830

Spreyermann Neurofeedback and Psychotherapy for C-PTSD
there was no further improvement due to the irregular training,
more intensive training was resumed. After 2 years, consecutive
new placements were added to T4P4, and now training on all
four basic sites is possible (T4-P4, T3-T4, T4-Fp2, and T3-
Fp1). Fp1-Fp2 training helps to reduce compulsive behavior and
racing thoughts.
In her own words, the patient asserts that before the
neurofeedback treatment, she had to take the strongest
medications and yet was unable to sleep well at all. Now, after 2–3
years of neurofeedback therapy, she sleeps more profoundly for
more hours and experiences a better sleep quality. She says that
she is no longer afraid of going to bed. In addition, she describes
that she feels her body again—where earlier she had a feeling of
numbness and her body had not been present in her thoughts.
An Overall Appraisal of Clinical Results
A quantitative appraisal of clinical effectiveness in the manner
of a formal retrospective study is not appropriate, given the
heterogeneity of the clinical population, as well as variety
of measures taken with each patient. However, looking back
qualitatively over the past 7 years, th e combination of trauma-
based psychotherapy and ILF neurofeedback has led to surprising
and motivating results.
For approximately 25% of the patients, there was an initial
improvement of the symptoms, but in the course of the therapy,
there was a stagnation of progress. In these cases, the addition or
adoption of other methods such as mindfulness training, HRV-
training, sports, or respiratory therapy should be considered.
In only 2 of 80 patients has there been no positive reaction to
the neurofeedback.
For around 15% of the cases, premature abandonment
of the t herapy was recorded, which can be traced to a
variety of reasons, which is common in the domain of
psychotherapeutic treatments.
However, for the rest of the patients with C-PTSD, good or
very good progress was observed. A n improvement of 60% up
to over 90% could be seen in symptom tracking, which is very
surprising given the severity of the initiating traumas and the
long-established symptom history of the patients.
Infra-low-frequency neurofeedback is emerging as a
promising method to help patients with PTSD. Both case
reports show that people who suffered a great deal and who
were not able to live a normal life were able to go back into
daily routines with the help of neurofeedback therapy. Even
though not all patients benefit, the strong likelihood of a positive
outcome is promising. One also must keep in mind that in
many cases, patients start neurofeedback therapy after having
already suffered a long time and having tried several therapies
without success.
DATA AVAILABILITY STATEMENT
The original contributions presented in the study are included
in the article/supplementary material, further inquiries can be
directed to the corresponding author/s.
ETHICS STATEMENT
Written informed consent was obtained from t he individual(s)
for the publication of any potentially identifiable images or d ata
included in this article.
AUTHOR CONTRIBUTIONS
The author confirms being the sole contributor of t hi s work and
has approved it for publication.
FUNDING
Open access fees are covered by the Brian Othmer Foundation,
6400 Canoga Ave., Suite 210, Woodlands Hill, CA 91367.
REFERENCES
Boscarino, J. A. (2009). Posttraumatic stress disorder and physical illness: results
from clinical and epidemiologic studies. Ann N Y Acad Sci. 1032, 141–153
doi: 10.1196/annals.1314.011
Cloitre, M., Garvert, D. W., Brewin, C. R., Bryant, R. A., and Maercker, A. (2013).
Evidence for proposed ICD-11 PT S D and complex PTSD: a latent profile
analysis. Euro. J. Psychotraumatology 4:20706.
Gerge, A. (2020a). What neuroscience and neurofeedback can teach
psychotherapists in the field of complex trauma: Interoception,
neuroception and the embodiment of unspeakable events in treatment
of complex PTSD, dissociative disorders and childhood traumatization.
Eur. J. Trauma Dissociation, 4:100164. doi: 10.10 16 /j .ejtd.2020.
100164
Gerge, A. (2020b). A multifaceted case-vignette integration neurofeedback and
EMDR in the treatment of complex PTSD. Eur. J. Trauma Dissoc. 4:100157.
doi: 10.1016/j.ejtd.2020.100157
Grunert, B. K., Weis, J. M., Smucker, M. R., and Christianson, H. F. (2007).
Imagery rescripting and reprocessing therapy after failed prolonged exposure
for post-traumatic stress disorder following industrial injury. J. Behav. Ther.
Exp. Psychiatry. 38, 317–28. doi: 10.1016/j.jbtep.2007.10.005
Imperatori, C., Della Marca, G., Amoroso, N., Maestoso, G., Valenti, E.
M., Massullo, C.h., et al., (2017). Alpha/theta neurofeedback increases
mentalization and default mode network connectivity in a non-clinical sample.
Brain Topogr. 30, 822–831. doi: 10.1007/s10548-017-0593 -8
Kimbrel, N. A., Wilson, L. C., Mitchell, J. T., Meyer, E. C., DeBeer, B.
B., Silvia, P. J., et al., (2017). ADHD and nonsuicidal self-injury in
male veterans with and without PTSD. Psychiarty Res. 252, 161–163.
doi: 10.1016/j.psychres.2017.02.015
Lake, J. H. (2015). The integrative management of PTSD: A review of conventional
and CAM approaches used to prevent and treat PTSD with emphasis on
military personal. Adv. Integr. Med. 2, 13–23 doi: 10.1016/j.aimed.2014.10.002
Lanius, R., and Frewen, P. (2015). Healing The Traumatized Self. New York,
London: W. W. Norton and Company.
Lanius, R. A., Frewen, P. A., Tursich, M., Jetly, R., and McKinnon, M. C.
(2015). Restoring large-scale brain networks in PTSD and related disorders:
a propos al for neuroscientifically-informed treatment interventions. Eur J
Psychotraumatol. 6,27313. doi: 10.3402/ejpt.v6.27313
Lanius, R. A., Nicholson, A. A., Rabinello, D., Densmore, M., Frewen, P. A., Paret,
C.h., et al., (2017). The neurobiology of emotion regulation in posttraumatic
stress-disorder: Amygdala downregulation via real-time fMRI neurofeedback.
Hum Brain Mapp. 38, 541–560. doi: 10.1002/hbm.23402
Frontiers in Human Neuroscience | www.frontiersin.org 5 May 2022 | Volume 16 | Article 893830

Spreyermann Neurofeedback and Psychotherapy for C-PTSD
Micoulaud-Franchi, J. A., Jeunet, C., Pelissolo, A., and Ros, T. (2021). EEG
neurofeedback for anxiety disorders and post-traumatic stress disorders: a
blueprint for a promising brain-based therapy. Curr Psychiatry Rep. 2384.
doi: 10.1007/s11920-021-01299-9
Othmer, S. F. (2017). Protocol Guide for Neurofeedback Clinicians. 5 Edn. Los
Angeles, CA: EEG Institute.
Othmer, S. F., and Othmer, S. (2017). Rhythmic Stimulation Procedures in
Neuromodulation, editors Evans, R.E. and Turner, R. A. San Diego: Academic
Press. p. 225–278
Panisch, L. S., and Hang Hai, A. (2020). The effectiveness of using neurofeedback
in the treatment of post-traumatic stress disorder: a systematic review. Trauma
Violence Abuse. 21, 541–550 doi: 10.1177/1524838018781103
Reiter, K., Andersen, S. B., and Carlsson, J. (2016). Neurofeedback treatment
and posttraumatic stress disorder: effectiveness of neurofeedback on
posttraumatic stress disorder and the optimal choice of protocol.
J Nerv Ment Dis, 204, 69–77 doi: 10.1097/NMD.00000000000
00418
Shapiro, F. (1995). Eye Movement Desensitization and Reprocessing (EMDR)
Therapy: Basic Principles, protocols, and Procedures. New York: Guilford Press
van der Kolk, B. A., Hodgon, H., Gapen, M., Musicaro, R., Suvak,
M. K., Hamlin, E., et al., (2 01 6). A randomizes controlled study
of neurofeedback for chronic PTSD. Randomized Controlled
Trial>PLoS. 11,e01166752. doi: 10.1371/journal.pone.016
6752
van der Kolk, B. A., Rogel, A., Loomis, A. M., Hamlin, E., Hodgdon, H., and
Spinazzola, J. (2020). The impact of neurofeedback training in children with
developmental trauma: a randomized controlled study. Randomized Controlled
Trial > Psychol Trauma. 918–929 doi: 10.1037/tra0000648
Wiedemann, M. (2020). Neurofeedback in Clinical Practice in Restoring the Brain,
Neurofeedback as an Integrative Approach to Health, ed. H. Kirk. 2nd edition.
Routeledge, New York. p. 56– 79.
World Health Organization (2022). ICD 11 for Mortality and Morbidity Statistics:
6B41 Complex posttraumatic stress disorder. Available online at: http://id.who.
int/icd/entity/585833559 (accessed February, 2022).
Conflict of Interest: The author declares that the research was conducted in the
absence of any commercial or financial relationships that could be construed as a
potential conflict of interest.
Publisher’s Note: All claims expressed in this article are solely those of the authors
and do not necessarily represent those of their affiliated organizations, or those of
the publisher, the editors and the reviewers. Any product that may be evaluated in
this article, or claim that may be made by its manufacturer, is not guaranteed or
endorsed by the publisher.
Copyright © 2022 Spreyermann. This is an open-access article distributed under the
terms of the Creative Commons Attribution License (CC BY). The use, distribution
or reproduction in other forums is permitted, provided the original author(s) and
the copyright owner(s) are credited and that the original publication in this journal
is cited, in accordance with accepted academic practice. No use, distribution or
reproduction is permitted which does not comply with these terms.
Frontiers in Human Neuroscience | www.frontiersin.org 6 May 2022 | Volume 16 | Article 893830
